Mammograms

Millions of women are surviving breast cancer today, thanks to early detection and improvements in testing and treatment. Mammogram screenings are the most effective method for the early detection of breast cancer. It is important to get the recommended screening tests before any symptoms develop. When cancer is found in the early stages, it is easier to treat. Caught early enough, breast cancer often can be cured. Women who are 40 years and older should have a screening mammogram every year as a regular part of their health care.
What is a Screening Mammogram?
A mammogram is an x-ray image of the breast. The x-ray images make it possible to detect abnormalities that cannot be felt during a physical exam or breast self-exam. These can help identify cysts, calcifications, and tumors within the breast before they are large enough to be felt, and are used to check for breast cancer in women who have no signs or symptoms of the disease.
In-Office Digital 3D Mammogram Screenings
We offer the ease and convenience of having your mammogram screening done in the office with the flexibility to schedule the screening the same day as your well woman visit.
Our advanced digital screening mammogram makes state of the art technology accessible to all women. Digital mammograms are electronic images of the breast, acquired at different angles, that can be enhanced, magnified, or manipulated for further evaluation, offering the following advantages over conventional mammogram:
- Health care providers can share image files electronically, making longdistance consultations between radiologists and breast surgeons easier.
- Subtle differences between normal and abnormal tissues may be more easily noted.
- Fewer followup procedures may be needed.
- Fewer repeat images may be needed, reducing the exposure to radiation.
Your screening mammogram will be performed by an experienced Registered Technologist and interpreted by a board certified breast imaging physician radiologist.
Some women are at higher than average risk for breast cancer and should talk with their physician about whether to have mammograms before age 40 and how often to have them.
Factors that increase a woman’s risk of breast cancer
- Age: The risk of breast cancer increases as a woman gets older.
- Personal history
- Family history
- Genetics: BRCA1, BRCA2, and other gene mutations.
- Breast density
- Early menstruation (before age 12)
- Late menopause (after age 55)
- Hormone therapy after menopause
- Pregnancy: Women who have had their first fullter pregnancy after age 30 or who have never had a fullterm pregnancy.
- Alcohol intake
- Being overweight or obese
You also may need a mammogram if you have any of these signs:
- Lump or thickening in the breast
- Swelling of all or part of a breast (even if no distinct lump is felt)
- Skin irritation, dimpling, redness, or other changes in the skin of the breast
- Nipple discharge or bleeding
- Nipple retraction (turning inward)
- Breast or nipple pain
If you should experience any of these signs, talk to your doctor about having a physical exam and mammogram.
Minimally Invasive Surgery
Is used to treat the following conditions:
- Irregular / Heavy periods
- Endometriosis

- Ovarian cysts
- Pelvic pain
- Pelvic prolapse
- Urinary incontinence
- Uterine fibroids
- Undesired fertility
Minimally invasive surgery allows surgeons to use special instruments in surgery that require either tiny incisions, or no incisions at all (hysteroscopy), to achieve the same surgical goals as a traditional “open” procedure.The instruments that are used are long, lighted scopes with attached cameras connected to a monitor where the surgeon has a 3D view. Many additional instruments may be used through these scopes to perform the type of surgery needed. This minimally invasive approach enables women to return to their daily activities
in less time and with less discomfort than with traditional surgery. Three of our surgeons: Dr Carducci, Dr Jones and Dr Durkee have been named designees of “Center of Excellence in Minimally Invasive Gynecology”. They are recognized Nationally for their high-quality, minimally invasive surgical skills and exceptional patient outcomes.
Some of our physicians perform minimally invasive procedures utilizing the daVinci Robotic system at the Winnie Palmer Hospital. The daVinci system utilizes advanced robotic technology that enables the surgeon to operate using high definition, 3D imagery with enhanced dexterity enabling more precise and controlled movements, all done through very small incisions. Patients experien
ce less pain, length of hospital stays and rapid return to normal daily activities. The robotic assistance generally is used for for complex procedures.
Some common major procedures performed by minimally invasive surgery include hysterectomies (removal of the uterus), removal of ovaries, myomectomies (removal of fibroids from the uterus while preserving the uterus) and pelvic organ prolapse surgeries. The surgery involves using the laparoscope which is a long lighted instrument introduced into the abdomen along with other instruments toperform the surgery. All movements are controlled by the surgeon at an operating console looking at magnified 3D imagery, through a high definition camera. The enhanced imagery helps to minimize blood loss and perform more precise dissections, ultimately providing ease of surgery for both patient and surgeon. Patient satisfaction is heightened by minimally invasive surgical approaches and we provide much support and education, as you plan any surgical treatment plans.
Ultrasound

Women’s Care Florida OB & GYN Specialists ultrasound program is accredited by AIUM (American Institute of Ultrasound in Medicine). We are able to offer both gynecologic and obstetric ultrasound services that are performed by specially trained ultrasonographers at all 3 office locations.
Traditional 2D ultrasound is what we use for most of our medical indications. This gives us the gray ultrasound picture that people are used to seeing. We use this type of ultrasound to look at the female organs such as uterus, ovaries, and fallopian tubes and we perform all pregnancy related medical imaging this way including pregnancy confirmation, Nuchal Translucency (NT) and fetal anatomy scans.
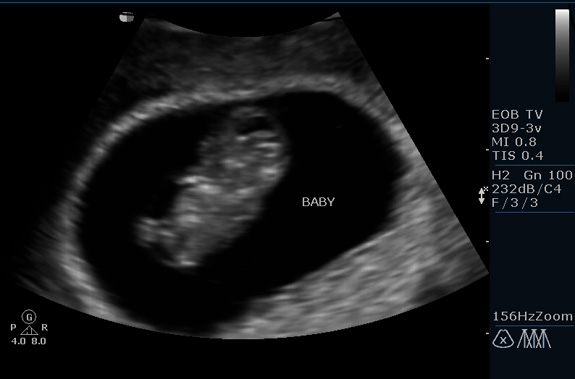
The exam can be performed transabdominally, but the patient must have a full bladder or be pregnant in order to be able to view the structures completely. We can usually get a better image transvaginally where we use a special transducer that is placed just inside the vagina. This exam is generally painless, and is performed by a female technician. All ultrasound rooms are equipped with monitors so that the patients can see the images as the tests are being performed.
Sonohysterography is a specialized procedure where sterile saline is installed into the uterine cavity, and an ultrasound is performed at the same time. The procedure helps to delineate intrauterine pathology such as polyps, fibroids and uterine malformations.
In-Office Surgeries
Women’s Care Florida OB & GYN Specialists offers several minor surgeries in our office thus avoiding the need for hospitalization. This saves time, cost and need for general anesthesia. Our office is “SCOPE” certified which is a stringent voluntary program designed to deliver the highest level of patient safety in outpatient surgery. We still perform the procedures in the hospital but with careful patient selection, they can be done safely in our office. This makes for a less stressful and more convenient patient experience. These procedures include:
- Endometrial ablation (both Minerva and Novasure)
- LEEP procedure
- Hysteroscopy
- Dilation and Curettage
- TruClear Hysteroscopic Resection
- EndoSee Hysteroscopy
Endometrial Ablation
This procedure involves the destruction of the endometrial lining of the uterus, used mainly to treat abnormal bleeding and to reduce menstrual flow. Heavy menstrual bleeding can cause significant changes in daily lifestyles such as anemia, exhaustion and depression. For women with heavy periods who cannot tolerate birth control pills, endometrial ablation is an option and alternative to hysterectomy.
We offer two types of endometrial ablation: Novasure and Minerva. These can be performed in our office using local anesthesia and pain medications. The procedures are short 5-10 minutes. Mild cramping and nausea can occur post procedure. An endometrial biopsy (a sampling of the uterine lining to rule out cancer) and an ultrasound should be performed prior to scheduling the procedure. These initial tests will help you and your doctor to decide which ablation procedure is best for you.
Ablation should not be done if pregnancy is still desired. You still need birth control after the procedure. Benefits of endometrial ablation include:
- High success and patient satisfaction rates
- No hormones
- No general anesthesia
- No hospital costs
- Short recovery time
- Decrease and possible elimination of menstrual flow
LEEP Procedure
If you have abnormal Pap test results, your doctor may suggest you have a Loop Electrosurgical Excision Procedure (LEEP). LEEP is one way to remove abnormal cells from the cervix by using a thin wire loop that acts like a scalpel. An electric current is passed through the loop which cuts a very thin layer of the cervix; local anesthesia will be used to prevent pain.
Hysteroscopy
A procedure used to diagnose causes of abnormal bleeding or to remove small polyps or intrauterine devices (also known as IUDS). A small scope is passed through the cervical opening and the uterine cavity is filled with fluid so the endometrial cavity can be seen. This can be done with local anesthesia.
BOTOX® Cosmetic
Botox stands for OnaBotulinum-Toxin-Type-A. We use it in the forehead area to diminish the cause of wrinkles which are a result of repeated contractions of the facial muscles. A small quantity of solution is injected directly into these muscles in multiple areas. Typically several injections are given with each treatment, and one treatment is usually effective for 3-4 months.

